|
"Physician Assistants (PA) are academically prepared and highly skilled health care professionals who provide a broad range of medical services. PAs are physician extenders and they work with a degree of autonomy, negotiated and agreed on by the supervising physician(s) and the PA. Activities may include conducting patient interviews, histories and physical examinations; performing selected diagnostic and therapeutic interventions or procedures; and counseling patients on preventive health care." - CAPA If you are in the Hamilton area, the McMaster PA Class of 2016 will be setting up booths in the following areas on November 27, 2014 between 9:30AM-4:00PM. Please come see us if you are interested about who Physician Assistants are.
If you're interested in the program itself, the PA Program information night is on November 26, 2014 at McMaster HSC 1A1 7PM. Join us on social media by following the hashtag #PADayCA !
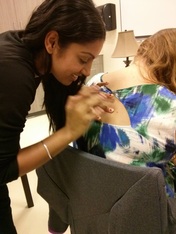 Longitudinal Placements (LP) are clinical observerships organized by the student in domain of his/her choice to gain relevant clinical knowledge in that area of medicine 1. What LP did you do? I did an LP with Hamilton EMS. 2. How did you go about contacting and arranging the LP? LPs with Hamilton EMS require a request from the Physician Assistant office, therefore, individual students cannot email the paramedics themselves and arrange an LP. I e-mailed Nancy Weller (PA program Manager) with three days I was available for 12 consecutive hours and we went from there. 3. What were the two main things you learned from the LP? I learned that paramedics have a wide range of responsibilities, and their scope of practice is also very broad. Not only do they provide life saving care but they can also give certain medications and take pertinent histories at the scene. Most importantly, contrary to the common misconception, paramedics are not "taxi drivers"! They provide a lot of life saving care at the scene before stabilizing the patient and bringing him/her to the hospital. I had the opportunity to listen to a murmur, learn how to interpret several EKGs, and I witnessed the protocol for a patient found with "absent vital signs" and in cardiac arrest. 4. What did you wish you knew beforehand to help you in your LP? I wish I had a better understanding of how to interpret EKGs. Every patient that we saw was put on an EKG machine, some of which had abnormal EKGs. However, the paramedics took time out (when possible) to teach me how to interpret EKGs. 5. How has this experience helped you clinically, in class and/or in career decision making? This experience has helped me understand EKGs better because I now have a real life situation to think about when learning about ventricular tachycardia or ventricular fibrillation. In addition, I also saw an angiogram in the emergency department and that experience has helped me understand the reasoning behind the need for an angiogram. In terms of career decision making, I learned that the emergency department is a very fast paced environment, one is always on their feet and ready to deliver optimal healthcare- this is of interest to me. 6. Any other comments? I strongly recommend that everyone go out for an EMS ride-out to gain a better understanding of the roles and responsibilities of paramedics. This is especially important if you want to work in the ER because you will be interacting with these health care professionals on a day to day basis. A firm understanding and appreciation for all their hard work will help foster a good relationship between the two professions. FUN FACT:
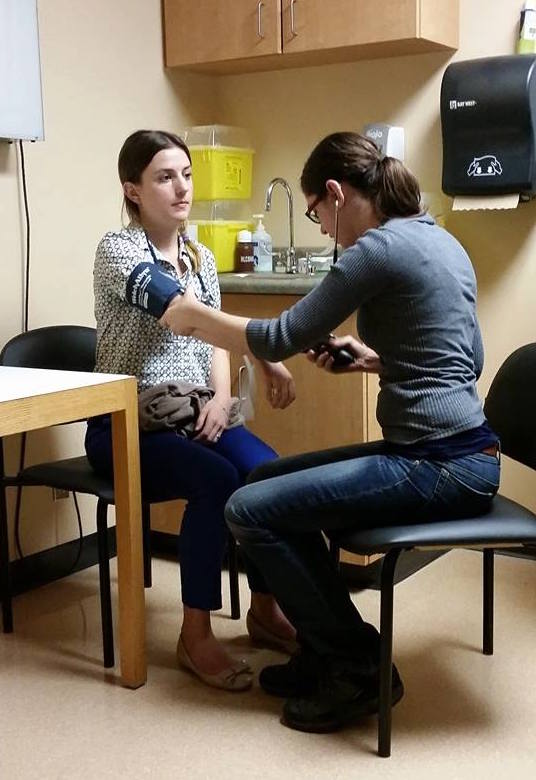
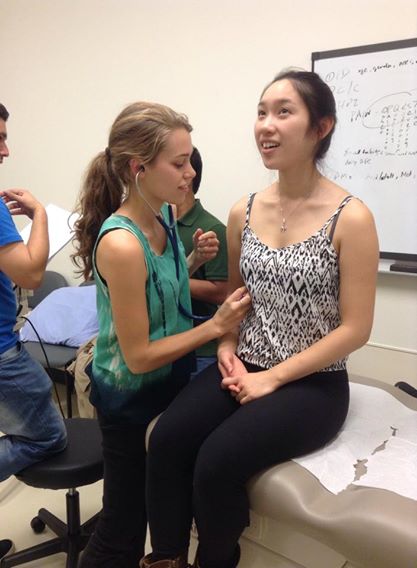
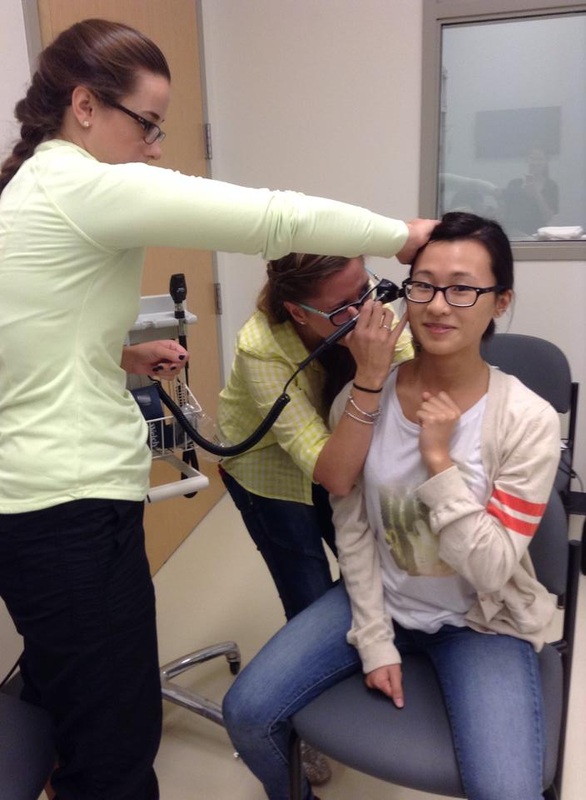
EMS service is NOT FREE. The Ontario Health Insurance Plan (OHIP) covers the majority of that fee, so patients are only billed $45.00. However, if the hospital/doctors determines that the patient could have made their way to the hospital by another means or the trip was not "medically essential", the patient will be billed for the full amount of the ambulance bill ($240.00). This is necessary in order to ensure that the system is not abused, and that the service is available to those who really need it! Took us a while to settle into the program but the Class of 2016 is now ready to share with you our experience in the PA program! We really want to show you what we are learning in the PA program and share our clinical experiences from our Longitudinal Placements (LP). This will allow you to get a glimpse of how the PA program is training us to become competent and compassionate Physician Assistants. We will also share information regarding who Physician Assistants are and how they fit in a health care team (National PA Day is coming up! #PADayCA) One of the classes we have is Interviewing, Examining, and Reasoning. In this class, we learn how to do the above three things. We started off with learning how to take vitals (eg. Blood Pressure, Respiratory Rate, etc). Then we practiced the Respiratory and Cardio exam.  One of the best ways to practice our clinical skills is on Standardized Patients (SP). SPs are actors who come in presenting us with a case. We approach and interact with each SP as if they are real patients. We were a bit nervous at first but getting the opportunity to practice our clinical skills on SPs really helped us!  Two weeks ago, we had our Operating Room Orientation at Juravinski Hospital. This consisted of a tour around the OR and being taught how to get our scrubs (via the ScrubEx Machine). On Halloween this year, a few of us had the amazing opportunity to hand out candy to kids staying at the McMaster University Medical Centre during the Halloween Parade. No pictures of the kids are allowed but we can assure you they are so cute in their costumes. This concludes the summary of what we have been up to the last two months! Follow us on our social media to stay connected (click the pictures to be redirected)! If you have any questions regarding the program or the profession, please do not hesitate to contact us at [email protected] or through our Facebook page.
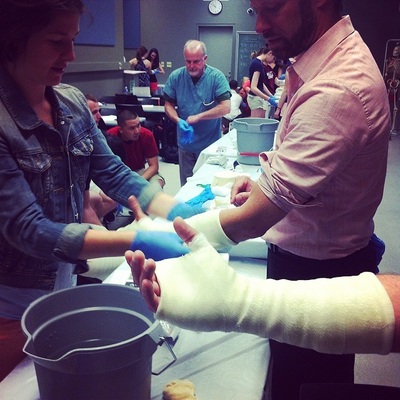
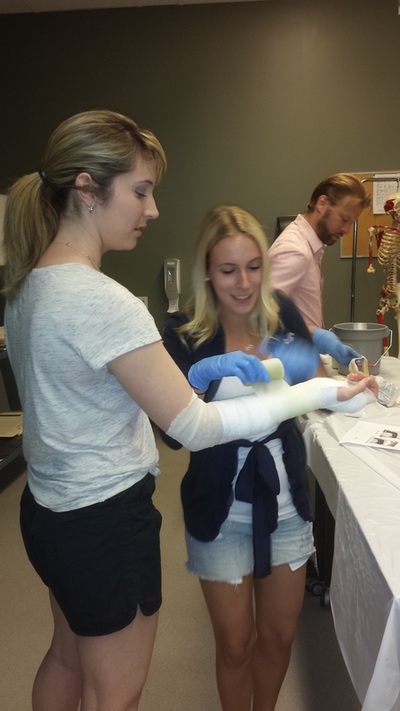
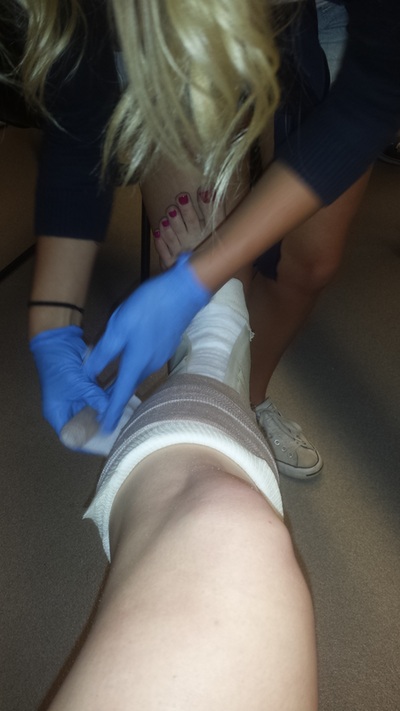
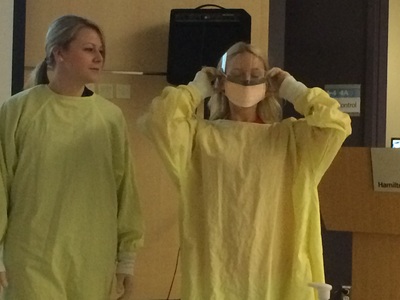
Don't forget, National PA Day in Canada is happening on November 27th, follow our hashtag #PADayCA!  What LP did you do? Of the 4 LPs I completed this year, my Hospitalist LP in Sault Ste. Marie, ON sticks out the most and was probably the biggest learning experience clinically that I had this year. How did you go about contacting and arranging the LP? I arranged this LP through the Sault Area Hospital (SAH) and Northern Ontario School of Medicine (NOSM) coordinators. They were happy to have me complete a longitudinal placement within their facility. What were the two main things you learned from this LP? There were many experiences I had while working with the Hospitalist team at the SAH. Two of those experiences that are at the top of the list would have to be: 1. Seeing how the multidisciplinary teams work together to accomplish the task of getting patients back into the community with the proper support networks. 2. How to successfully navigate and work in a hospital. How has this experience helped you clinically, in class and/or in career decision making? I was able to see how social work, OT, PT, nurses and physicians go about treatment plan goals and discharging the patient. While being with the Hospitalist team, I was permitted to see patients on the wards, in the ER and in the Psychiatric areas of the hospital. Working with this type of team enabled me to see different areas of the hospital as well as become familiar with computer systems and proper documentation of patient encounters. I completed two rotations with the Hospitalist team in SSM: one during Christmas and the other during March break. Although I had very limited training for my Christmas rotation, and months later in March I still lacked certain medical knowledge, these placements made me realize how valuable Problem Based Learning (PBL) is for continuing to develop your skill set as a PA. PBL gave me the tools to efficiently and effectively research specific medical topics as they pertained to the patients with which I was interacting which facilitated and maximized my learning experience. 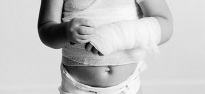 What LP did you do? I did my LP with a Physician in a Child Maltreatment Assessment Program. How did you go about contacting and arranging the LP? At our Interprofessional Education Day I met the head of the program and started chatting with her about pediatrics and her maltreatment assessment program. I asked if I could do an LP with her and she was very excited to have a PA since they had never had one before. She gave me her e-mail and phone number and we coordinated weekly half days for 4 weeks. What were the two main things you learned from this LP? 1. How one approaches the various assessments. For example the physical exam, observing family interactions, interviewing parents, and debriefing with the team. Also always keeping an OPEN mind. 2. How a multidisciplinary approach is very important, particularly in this domain. I was able to observe the interaction between pediatricians, psychologists, nurses, and child life specialists (I had never met one before so this was VERY exciting!). What did you wish you knew to help you in your LP? We had not done our psychiatry unit yet and I think that would have helped when sitting in on interviews to understand the types of questions asked and the flow of the interview. Also being familiar with the different types of maltreatment (physical abuse, sexual abuse, emotional abuse, and neglect), the warning signs, and the major repercussions would have helped a lot. How has this experience helped you clinically, in class and/or in career decision making? This experience showed me how to go about addressing such a touchy subject in clinical practice, as I was able to see the different approaches taken by each of the staff. I think it also helped emphasize the importance of a humanistic approach to healthcare, which can sometimes be forgotten when you are pulling your hair out trying to understand the pathophysiology of the illness with which you are presented. I was also able to see how Children’s Aid Society referrals worked, meeting a few case workers throughout the observership. I found this helpful because we discussed it briefly in our Professional Competency class, but I think it is something you should be comfortable with for practice. Any other comments? I have always been fascinated with children and I love their brutal honesty and humor. One of the main reasons I wanted to do this LP was to see if I was able to handle the challenging, serious and sad side of pediatrics. The cases were definitely heartbreaking, but this group works hard to help children escape these incredibly vulnerable situations, and that to me was the most amazing thing to witness. Hi everyone, I wanted to post about some of the things the PA class of 2015 got up to this year as a way to hype up the class of 2016. We've been trying to document the fun things we have done in class through Instagram, Twitter and Facebook, but I thought it would be nice to have a blog entry to reminisce about the memories and give the class of 2016 some things to look forward to. I remember my first day of PA school vividly; a wise man heavily involved in the PA program told me this: "In these next two years, you will meet your best friends; friends, colleagues and comrades that you will have for the rest of your life". He was so right about that! I am fortunate to have met a group of driven, intelligent and compassionate individuals. Here are a few snap shots of the time we spent together both inside and outside of class! Enjoy, Jessica O. Operating Room orientation and scrub session McMaster Homecoming game, 2013 Halloween gathering, 2013 Suturing (on pig carcass and sponges) IER workshop, 2014 Casting IER workshop, 2014 Infection Control and Prevention workshop, St. Joseph's Hospital, 2014 Ugly Christmas sweater get-together, 2013 IV skills IER workshop and Intubation workshop on Pediatrics Day Toronto Blue Jays game, McMaster Medical School formal (thanks for inviting us!), PA intramural soccer team! OSCE Day! June 2014
Funding available for Ontario non-Family Health Team, Family Medicine Physician Assistants7/22/2013
Dear PA stakeholders:
There is now a call for the groups of family doctors who are not in Family Health Teams to apply for permanent 100% funding to Allied Health providers, including Physician Assistants. Please see the message below from the Ontario Medical Association: Interprofessional Health Provider Funding Application Packages Now Available To: Primary Health Care Patient Enrolment Model Groups The 2012 Physician Services Agreement includes a provision for funding to support the integration of interprofessional health providers into non-Family Health Team affiliated patient enrolment model groups. The Ministry of Health and Long-Term Care will provide full salary funding to non-FHT affiliated PEM groups to promote the building of small interdisciplinary and collaborative teams to enhance access to and delivery of quality primary care within their communities. The application information package is now available online for member reference: http://www.health.gov.on.ca/en/pro/programs/ihp The deadline to submit applications is August 16, 2013 at 5 p.m. Groups selected to receive funding will be advised no later than September 16. If you have any questions or require additional information regarding this initiative, please contact the Ministry via email ([email protected]) or telephone (613-536-3219), or the OMA at [email protected] or 1-800-268-7215. Thank you. (via University of Toronto PA program's Facebook page) Be sure to take a look at the newest sections to our website:
Prepping for Your First Year of PA school Canadian Association for Physician Assistants - Membership Info The class of 2014 worked diligently to gather all the information included in these sections in order help incoming students better prepare for their first year in the McMaster PA program. Let us know what you think and if you have any ideas for the site leave us a comment!! 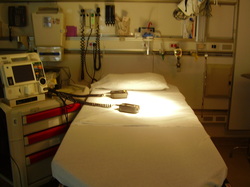 First year student Matt had a really great experience observing a trauma team earlier this year. Keep reading to learn more about what Matt got out of this placement. What LP did you do? I was with a trauma service! How did you go about contacting and arranging the LP? At a MacMed Trauma Interest Group event, I met a 5th year emergency med resident doing their fellowship in trauma. I asked if I could follow them around to learn about trauma, and they said why not! So I emailed them to get their availability and shadowed them after that. What were the two main things you learned from this LP? 1. Trauma is awesome and really interesting (there’s a lot of neurology and musculoskeletal stuff involved in trauma) 2. The whole trauma team is really diverse and you can see the whole interdisciplinary team in action; the team consists of an emerg doc, a general surgeon, an orthopaedic surgeon, a neurologist, an anaesthesiologist, nurses, among others. What did you wish you knew to help you in your LP? Ideally, I would have finished learning about neurology and MSK before jumping into trauma. I had no background in anatomy so I didn’t have a strong understanding of all the broken bones or affected brain structures that patients presented with. Nevertheless, it definitely sparked my interest in learning about MSK and neurology in the future, as I found that when I finally started learning about the material, it was fascinating, since I saw it in real life already. How has this experience helped you clinically, in class and/or in career decision making? As I mentioned earlier, it definitely helped me connect the content I was learning in tutorial to real life situations I’ve encountered already with the trauma service. It made learning a lot more interesting and memorable. In terms of career, I think it solidified my interest in emergency medicine, trauma and surgery. I’m definitely hoping to end up on one of these paths in the future! Any other comments? Trauma is cool for sure -- but in Hamilton, it’s unlikely to see any of the crazy stuff that you see on TV (gunshot wounds and such). More often, there’s blunt force trauma, falls off high places, MVCs (motor vehicle collisions), stabbings, and other miscellaneous things. Overall, it’s fascinating to see how cool, calm and collected the trauma team is at handling emergent situations.  I've had this little gem about Maitry's experience with some local midwives in my files for awhile...sorry for the delay, but enjoy! :) What LP did you do I did my LP in midwifery How did you go about contacting and arranging the LP? After a “Labour and Delivery” session with a midwife, I signed up with her and she emailed me within a month with the potential dates and timings for my LP. Then I stayed in touch with the secretary at the midwifery clinic and arranged the dates. What were the two main things you learned from this LP? First of all, I learnt the role of midwives in our healthcare field. Being completely unaware of their scope of practice, it was a great introduction for me. I observed two midwives and realized how involved they were with each mother-to-be and her partner. Secondly, I learnt the importance of communication with patients. Women going through various stages of pregnancy displayed a range of emotions, and had many concerns; yet they were just so happy to be going through this phase of their life. Compassion and empathy were integral to working with each mother-to-be/mother. What did you wish you knew to help you in your LP? I wish I had known a little bit more about fetal ultrasound and physical examination of fetal head. When I saw the first pregnant woman, I was very scared of hurting her and/or the baby. The midwife taught me the correct techniques and I feel a little more competent. How has this experience helped you clinically, in class and/or in career decision making? I have always been interested in OB/GYN and I am doing an elective next year with an obstetrician and a gynecologist. I feel that spending time with midwives has exposed me to the types of tests that are performed at different stages of pregnancy, common questions and concerns of expecting mothers, and patient education. I am now looking forward to my OB/GYN elective next year! Any other comments? I absolutely loved my placement! We are not exposed to a lot of OB/GYN cases and it is not a mandatory rotation during clerkship either. I would highly encourage those interested in OB/GYN, or those who would like to know more about this profession and how it fits in with healthcare, should definitely do an LP. |
ARCHIVES
May 2019
Categories
All
|




























 RSS Feed
RSS Feed
