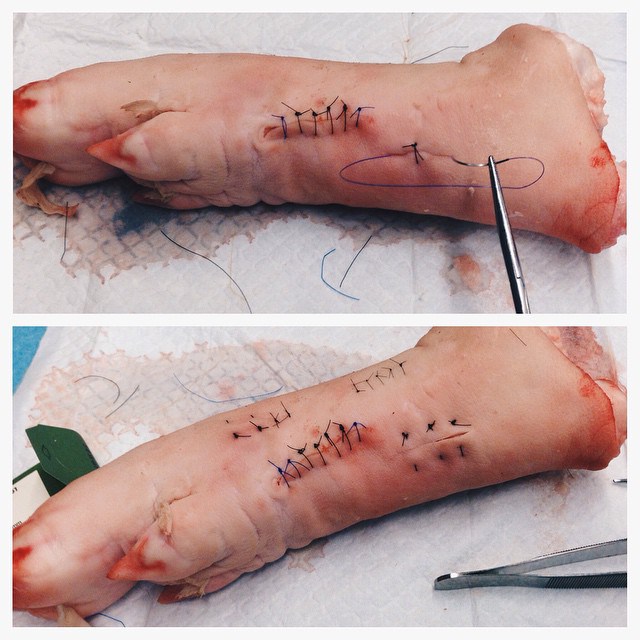
 Emma Wallace (current MPASA President) goes through the ins and outs of her longitudinal placement in infectious disease. What LP did you do? I did an LP in Infectious Diseases at Michael Garron Hospital (previously known as Toronto East General Hospital). How did you go about contacting and arranging the LP? Every student in the PA program is assigned a Student Advisor. Student advisors are practicing PAs who are responsible for mentoring 1-2 students in the PA class. At the beginning of the year, I met with my advisor and we discussed which areas of medicine I would like to do LPs in. My mentor was able to give me the name of an Infectious Disease PA working in my hometown. I emailed her and went from there! What were the two main things you learned from the LP? Infectious Diseases is a "consult service". This means that other medical specialties recruit the ID team when a patient has an infectious disease or an underlying infection that is challenging to treat. I got to see patients in general medicine, post-surgery, and in the emergency department. ID is an exciting medical specialty as clinicians get to be involved in a variety of different medical settings. It is important to educate patients about how to take antibiotics properly. The ID team sees patients who have infections that are very difficult to treat. Occasionally, this is because the source of their infection is resistant to most “good” antibiotics. Clinicians can do their part to mitigate this issue by prescribing antibiotics appropriately and educating their patients about how to take them properly. What did you wish you knew beforehand to help you in your LP? I wish I had known how to use the charting system in the hospital. Most people will feel this way during their first LP! It is one of those things that you just have to “learn by doing". Everyone has to start somewhere. How has this experience helped you clinically, in class and/or in career decision making? Infectious diseases affects many body systems, so I learned a lot on this LP. I also believe that this LP will come in handy in clerkship – in my internal medicine, surgery and family medicine electives I will likely be consulting the ID team or applying relevant knowledge.  Obligatory Scrub Selfie! Obligatory Scrub Selfie! Longitudinal Placements (LP) are clinical observerships organized by the student in the domain of his/her choice to gain relevant clinical knowledge in that area of medicine. What LP did you do? I did an LP in Plastic Surgery at McMaster University Medical Centre. How did you go about contacting and arranging the LP? I met a Plastic Surgery resident who helped me set up an LP with a plastic surgeon. The process of setting this LP up was really difficult because there was a lot of pre-placement work to be done: OR security access, OR orientation, Scrub Session, etc. What were the two main things you learned from the LP? 1. In my LP, I saw burn patients and patients post-op follow ups in the clinic; mastectomy for gynecomastia and surgery for syndactyly in OR; Basal Cell Carcinoma removal in minor procedures. Before my placement, I asked the surgeon's secretary for a list of surgeries he will be performing that day so that I can read up on them beforehand. It definitely helps to be prepared. Surgical procedures are usually reserved for last resort so when reading about the cases, I focused on why this patient is going in for this surgery/procedure and what indications did the patient have that surgery was suggested for treatment. 2. I learned the proper names of tools and how to use them (there's quite a few). I had the opportunity to assist the resident as well. He showed me how to cut sutures at an angle to avoid the knot and different types of sutures/patterns. The surgeon also took a bit of his time to explain local anesthesia to me. What did you wish you knew beforehand to help you in your LP? Operating Room Etiquette! I had to do an OR Orientation and Scrub session before my first placement so I really only know how to properly scrub in. I wish I knew that it's OR etiquette to get my own gloves, to help get the bed when the patient is ready to leave OR, etc. I also wish I practiced putting on sterile gloves in the absence of a scrub nurse and sterile gown. It's a challenge! TIP: Make sure the Avagard on your hands is DRY before putting gloves on, or else your hands are NOT going to go in. How has this experience helped you clinically, in class and/or in career decision making? The surgeon allowed me to scrub in so I had a lot of hands-on experience. I really liked my experience in plastics! The OR skills I learned are all transferable. I definitely got to see the surgical side of treatment. Congrats to the #PAClassOf2016 for completing their first year OSCE and the PA Class of 2015 for completing their second and LAST OSCE in the program!! OSCE stands for Objective Structured Clinical Examination. The stations are similar to the Multiple Mini Interview where there's a stem on the door and someone in the room whom we interact with. In the McMaster PA program, there are two OSCEs: one at the end of first year and the other at the end of second year. Second-Year PA students: "Are we PAs yet?" Pre and Post OSCE faces:
Good news! MPASA have organized and put together PA sweaters for students. It comes in maroon and grey with an option to personalize it on the right sleeve. These sweaters were ordered through a third party company and therefore is not available at McMaster bookstores. The sweater is a zip up hoody, perfect for wearing it over scrubs when it gets a bit chilly.
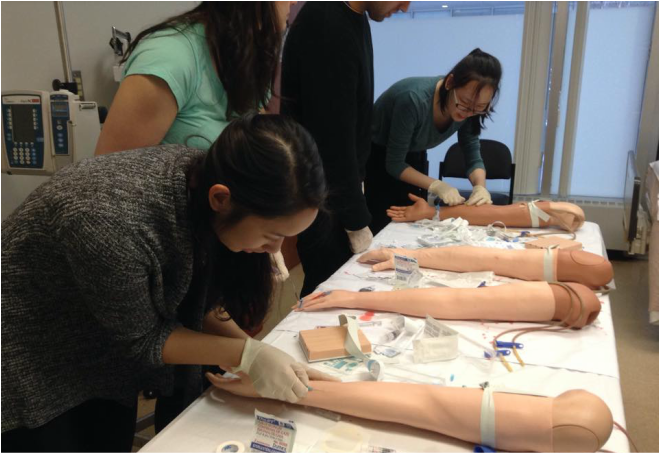
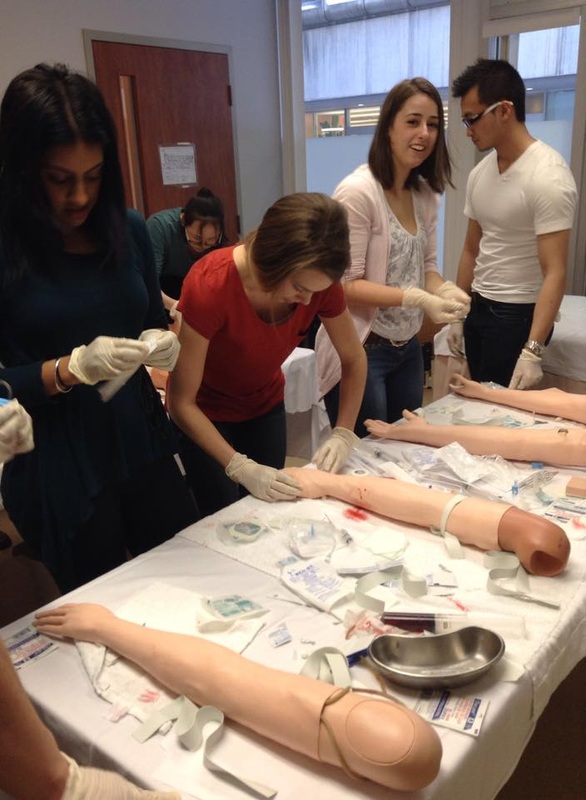
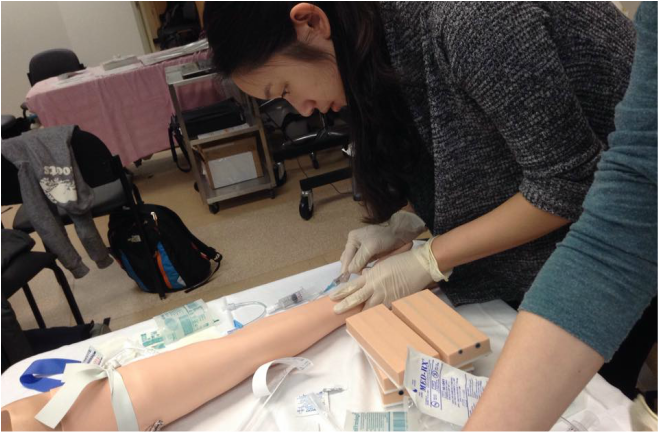
The logo design is taken from MPASA's logo (see right) and is embroidered onto the left chest. It has been a month since coming back from Christmas break and Medical Foundations 2 has been absolutely busy! We were told that it is only going to get busier. In this post, we want to share some things that have happened these past two months. IER WorkshopsAs part of our Interviewing, Examining and Reasoning (IER) course this term, we had an IV skill workshop and wound suturing workshop. We have already covered preforming a digital rectal exam and later on this term, we will be learning how to perform a female pelvic exam. Social EventsTime really flies by! We are already half way through the first year of the PA program. Although studying is important, spending time with our classmates outside of our tutorial group is just as important. Next year, we will be in different places for our clerkship, so it will be very difficult to hang out in a big group. Below are some photos of things we did as a group. We hope that this can help next year's incoming class to plan a few social events to facilitate group bonding.
Longitudinal Placements (LP) are clinical observerships organized by the student in domain of his/her choice to gain relevant clinical knowledge in that area of medicine What LP did you do? I did an LP in the Emergency Room at Norfolk General Hospital. It is considered a rural hospital with 106 beds to serve about 65 000 residents. How did you go about contacting and arranging the LP? I arranged this LP with the help of my Student Advisor. She referred me to a PA who is practicing in the Norfolk ER, and I was able to spend two 8-hour shifts in the emerg. It was great to see exactly what PA's role would be in an ER setting. What were the two main things you learned from the LP? This LP allowed me to understand how an ER functions and recognize some of the challenges that rural hospitals face. For example, rural hospitals have their own set of special populations that they need to address, and they have to be especially aware of the resources that are available to them in the area. There is also a great deal of inter-hospital collaboration to allow for more specialized care for patients. I was also able to observe and be involved in a bunch of procedures, like suturing, casting, INDs, and cardioversion. It was especially exciting to actually get to see the procedures you learn about in tutorials and textbooks in practice! What did you wish you knew beforehand to help you in your LP? I wish I had a few a more physical examination skills so that I could have been more involved in the patient interaction process. How has this experience helped you clinically, in class and/or in career decision making?
Before this experience, I was not familiar with what exactly goes on in an ER. This experience allowed me to understand exactly what kind of patients are managed, and how important it is to have good inter-professional relationships to ensure things run seamlessly. Any other comments? This LP was a fantastic opportunity to get a feel for a health care setting and to understand the role of a PA within it. My preceptor and the staff at Norfolk were all very encouraging and supportive, and being at a smaller ER made the space seem much more manageable than an urban hospital might be. That being said, I would most definitely like to go back once I have learned a bit more so that I can be involved more independently next time!  Longitudinal Placements (LP) are clinical observerships organized by the student in domain of his/her choice to gain relevant clinical knowledge in that area of medicine What LP did you do? I did the Hamilton EMS ambulance ride-along 12 hour shift. How did you go about contacting and arranging the LP? Contacted Nancy Weller who provided me with the paperwork required by Hamilton EMS to arrange date. I gave Nancy 3 dates that I was available to do the shift, and shortly after she gave me my shift date and time. What were the two main things you learned from the LP? It gave me a new perspective of the first response team and how important their role is in health care. I also learned how a patient's condition is coded (code 4=Lights on!) and how dispatch communicates with the paramedics to make sure that they are cared for as quickly as possible. What did you wish you knew beforehand to help you in your LP? Although what you encounter during any given shift is unknown (so you could be busy the full 12 hours or be waiting around for half the day), I did have a period of about 2 hours that we were waiting at the base, so I wish I had brought more reading material or study notes. Also make sure to bring food and layers if you are doing it during the winter. How has this experience helped you clinically, in class and/or in career decision making? It was great to communicate with patients and get a better perspective of the interaction between health care providers and the patient. As a future PA, the opportunity to work in first response is limited but it did give me insight in what it would be like to work in the Emergency room. It made me excited for my upcoming ER placements. Share your most memorable experience from the LP! My most memorable experience was when we were on stand-by at a fire, it was really cool to go on the other side of the yellow tape and see how all teams (police, paramedics and firefighters) work together in response to a disaster. Also, I enjoyed hearing all the interesting stories and experiences the paramedics had. Any other comments? I would highly recommend that everyone try a ride along at least once! Although it was a long shift it provides a unique experience that allow us to see what happens before the patient arrives at ER. What LP did you do? Juravinski Hospital Intensive Care Unit How did you go about contacting and arranging the LP? My preceptor is a tutor for the Med students; I was recommended to shadow this person by some Med students, and obtained his contact information from them. I reached out via email, explained that I was a first year Physician Assistant Student from McMaster looking to do an LP, and indicated the general time line I was looking to shadow him. He replied back with his availability, and we went from there! What were the two main things you learned from the LP? 1. How the ICU functions both as its own department, and with the rest of the hospital. I had the opportunity to follow the ICU routine from handover to rounds (note taking and orders) to procedures to family meetings. I was also able to attend a new patient consult, and learn how (and why) the ICU becomes involved in inpatient care. 2. The details around ventilation and the “go-to” ICU antibiotics. I hadn’t really spent much time thinking or learning about this on my own, and since both of these things were a big part of each patient’s care, it was a great opportunity to learn more about them! What did you wish you knew beforehand to help you in your LP? All the short forms and “nicknames” the staff had for diseases, procedures, and medications! On the first day, I found it hard to follow along with the fast-paced rounds with all the jargon flying around. However, all team members were open to chatting about things afterwards, and I found looking stuff up on my own before I came in the next time to be helpful. How has this experience helped you clinically, in class and/or in career decision-making?
The first thing that struck me was how each bed seemed to be a different MF1 case. It was very interesting and helpful to see these cases in real-life. This placement also demonstrated the importance of trying a wide variety of different LPs before settling on an area of medicine. While you might have something particular in mind, trying it (and other fields) out will provide invaluable insight for future career and elective decisions! Share your most memorable experience from the LP! I was able to sit in on several family meetings (family members of an incapacitated patient and the medical staff gather to discuss care options). The differences in level of understanding and socioeconomic status between families were striking. It really emphasized the importance of being a good communicator, by being able to adjust your explanations according to the audience. Presenting a caring, yet informative, persona was imperative for every patient/family encounter. While communication skills might not be everyone’s favourite class, it really is one of the most important – what good is knowing all the pathophys or clinical guidelines if you can’t communicate it to those who need to know? Time in the ICU really highlighted the importance of this skill, as your ability to communicate will dictate the care your patients actually receive. Any other comments? If you do any sort of ICU, or other ward, placement, I would recommend staying for the whole day, or coming in at different times if you can only commit a half day at a time. Things operate very differently in the morning compared to the afternoon. And sometimes things come up (e.g. new consult) that requiring deviating from the original plan. Also, come up with some learning objectives before you do any placement, and share these with your preceptor. These will help focus your learning in an overwhelming environment, where the learning opportunities are everywhere! On November 28, I had the wonderful opportunity to attend an event at the Six Nations Reserve, hosted by the Aboriginal Student Health Sciences (ASHS) Office. "Come Explore Health Careers Day" was an opportunity for various medical professional students at McMaster University to provide Grade 8 students at the J.C. Hill School in Ohsweken, ON, exposure to a variety of health careers. Our group consisted of 15 students from Medicine, Nursing and myself! I was super excited to work McMaster students from the other faculties, understand more about their roles, and share the role of Physician Assistants in medicine and health care teams. We began our day by handing out awesome T-shirts to all the Gr. 8 students, which were designed by some lovely folks at ASHS. This was followed by an icebreaker with the Gr. 8 students that led us to discuss the roles of medical professionals such as physicians, physician assistants, nurses, midwives, OTs, PTs. I was pleasantly surprised that these students had a great understanding of the roles played by most of these professions!Ear Traditional MedicineThe icebreaker was followed by a presentation from an Elder of Six Nations, who spoke to the group about Traditional Medicine. I was so impressed with her presentation because she molded Aboriginal values with the use of medicine, while placing great emphasis on expressing emotions such as hurt, grief and anger. My favorite part of this session was when she described the importance of giving hugs to one another! She said, "It is important for our hearts to touch and that in itself is a form of medicine". I strongly believe that teaching affection and care to pre-teens is extremely vital to their development and success as teens and adults. Engaging Clinical Activities The rest of the afternoon was broken in to 4 sessions through which the students rotated: Infectious Disease, Sign/Symptoms of Myocardial Infarction (Heart Attack), Cardiothoracic Anatomy and Clinical Skills. These stations allowed us to teach students about the importance of hygiene and preventing the spread of disease; identifying the signs and symptoms of community members experiencing a heart attack; hands-on exploration of pig pluck (heart, lungs, trachea); and common medical skills. I had the fortunate opportunity to be involved in this latter station where we showed students how to use a pen light to check pupillary reflexes. We also had some great laughs using tongue depressors in each other's mouths (the uvula totally freaked them out while making them giggle at the same time!). We also used the pen light to look into each other's noses (mainly mine!). One of the med students and I took turns showing the kids how to use blood pressure cuffs and measured blood pressure on all of us. The nursing students had set up an AMAZING Wound Care station by simulating lacerations on butternut squash! The students were absolutely fascinated by this station and learned to drape and cover large cuts. Spreading Awareness about Physician AssistantsNot only did I get to show these students the cool clinical skills we've acquired so far, I was also able to engage discussions about the role of PAs with both the medical school students as well as the nurses. Both nursing and medical students were quite curious about our profession - they had some great questions and we had lengthy conversations about the education of PAs, our capabilities and our place in the health care system. Furthermore, gaining exposure to life on the reserve was such a valuable experience. Get Involved in Spring 2015The Six Nations Reserve is about a 40-minute drive from campus and there are multiple university groups that are connected with the reserve through research, medicine and education. I would absolutely recommend getting involved in any of these ventures because they help us gain a better understanding of Native culture, traditions, as well as health care and educational issues specific to reserve life. During the spring of 2015, the ASHS Office will be holding an educational seminar on campus to expose Grade 12 students from the reserve to the different medical programs available at McMaster University. This would be a great opportunity for the PA program and our class to get involved!
Fun Fact: Earlier that afternoon, the 403 EB (Toronto) experienced a mudslide, which caused a lot of chaos all around the university - there was massive blockage of all roads in and out of the university, Westdale, Ancaster, Dundas and Cootes. The mudslide was caused by a burst water pipe but thankfully no one was hurt! Longitudinal Placements (LP) are clinical observerships organized by the student in domain of his/her choice to gain relevant clinical knowledge in that area of medicine 1. What LP did you do? I did an LP in the Emergency Room at Sunnybrook Hospital in Toronto. 2. How did you go about contacting and arranging the LP? Maureen Taylor is my preceptor for ProComp and she also works at Sunnybrook Hospital as a Physician Assistant in the ER. I emailed her and we were able to set up an LP. 3. What were the two main things you learned from the LP? I really enjoyed the time I spent in the ER because I learned a lot about the structure of patient care in a busy, level-one trauma centre. It was really useful to learn how a PA functions within the ER team. I was able to observe several procedures. 4. What did you wish you knew beforehand to help you in your LP? If I were to go again, I would like to read up on common medications used in the ER and their MOAs. 5. How has this experience helped you clinically, in class and/or in career decision making? Being in the ER helped me bridge my understanding of history-taking and physical exams from the classroom to a clinical setting. 6. Any other comments? I would recommend it to my classmates and I would love to try another LP in the ER! Maureen Taylor, CCPA, McMaster PA Class of 2010Prior to becoming a Physician Assistant, Maureen worked as a medical journalist and television reporter for the CBC for two decades. She is currently working as a PA at Sunnybrook Hospital in the Emergency Department. She is also a preceptor for the McMaster PA Program Professional Competencies class.
Follow her on Twitter @maureentaylor31. Read more about Maureen here: http://www.thestar.com/life/health_wellness/2010/11/19/cbc_health_reporter_graduates_as_physician_assistant.html |
ARCHIVES
May 2019
Categories
All
|




















 RSS Feed
RSS Feed
